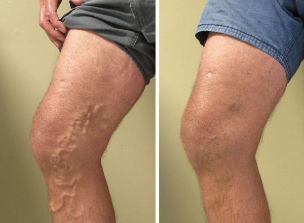
Varicose veins are a disease characterized by changes in the condition of the veins in the legs with impaired blood flow. If the shape is neglected, the blood vessels bulge, leading to swelling and pain in the limbs (under load) as well as aesthetic discomfort. Surgical removal of damaged veins is effective at this stage.
Indications for varicose vein surgery
Varicose vein surgery should only be performed if there are signs that the blood vessels have been removed:
- varicose veins affected most of the vein;
- severe pain and swelling of the legs during physical exertion that interferes with a normal lifestyle;
- development of open wounds and ulcers in the background of the development of the disease. It is dangerous to bind a secondary infection;
- Violation of blood permeability through blood vessels, often accompanied by convulsions;
- significant development of vascular necrosis;
- Pathological changes in the veins, along with their extent and prominence. The change is dangerous due to damage to the vessels and also causes aesthetic discomfort;
- blood clots in the blood vessels.
Surgery is only allowed with advanced forms of varicose veins and, in the absence of dynamics, conservative treatment.
Absolute and relative contraindications to surgery
Varicose vein removal surgery is performed not only in indications but also in the absence of contraindications:
| Absolute disabling of the operation | List of relative bans |
| Stable high blood pressure | Presence of infectious diseases |
| Blood pressure jumps regularly | Dermatological pathologies affecting the skin of the feet |
| Chronic heart disease | Inflammatory processes in the body, including blood vessels |
| Advanced age after 70 years | Recovery period after other surgeries |
| Presence of tumors | Chemotherapy |
| Diabetes and severe asthma | Severe soft tissue injury from trauma |
| Thinning and fragility of blood vessels | Liver and kidney disease in the acute stage |
| Patients with limited leg movements (paralysis) or bedridden patients | Blood clotting disorder or anemia |
| Returns to the last section | Taking hormones, antibiotics, or other hard medications |
| Complex leg fractures (with damage to blood vessels and nerve endings) | Overweight |
| Allergic reaction to medication used during surgery | Patient refuses surgery |
Carrying a child also affects the condition of the veins in the leg. More often, the pathology resolves on its own after delivery. In the presence of contraindications, surgery is dangerous with deterioration of the patient's condition and even fatal outcome.
Phlebectomy
Phlebectomy is a surgical procedure to remove damaged veins and restore normal blood flow to deep veins.
Anatomical meaning and technique of major vein removal surgery
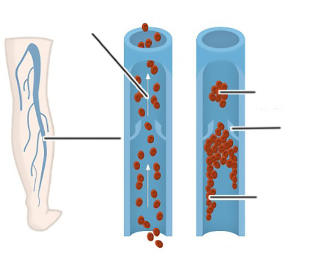
The circulatory system of the legs consists of a deep vein and several branches of the superficial veins that act on the varicose veins. Changes in vascular activity are due to valve malfunctions. During normal blood vessel function, the valves are closed, which allows blood to flow in only one direction.
In the veins affected by varicose veins, the valves do not close, as a result of which the blood can move in both directions, leading to impaired blood flow, with blood clots and protrusion of the veins.
In order to restore the blood supply to the limb, the affected vein must be removed (with reverse blood flow), ie a phlebectomy must be performed. Before the operation, the patient undergoes preparation (making tests, examining the condition of the veins, determining the general condition of the patient).
If there are no contraindications, specialists will perform a surgical procedure consisting of the following stages:
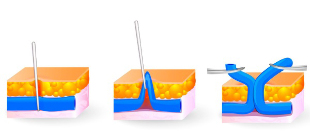
- Access to the affected vessel can be achieved through a small incision (in the groin or popliteal, depending on the location of the vein). The damaged blood vessel is then ligated from a deep vein to block blood flow.
- An incision is made near the varicose vein. Using a probe, the blood vessel separates from the muscle tissue, lymphatic system, and small capillaries. The damaged vein is removed through a tube or a hook.
- Capillaries are used to prevent bleeding.
- If there are damaged capillaries that form poker, they will be removed.
- At the end, cosmetic stitches, a disinfectant bandage and an elastic bandage are applied.
The operation is performed under general or local anesthesia. It depends on the size and location of the pot.
Efficiency level
Surgical removal of veins is used at different stages of varicose veins. The procedure is extremely efficient (more than 98%). The blood circulation is restored in a short time.
Rehabilitation
The effectiveness of the procedure depends not only on the surgeon's qualifications but also on compliance with the rules in the postoperative period.
After phlebectomy you need:
- suture care for 7-14 days in hospital;
- wears compression stockings or elastic bandages for 30 days all day;
- After 30 days, for another 3 months, wearing special underwear during the day
- aqueous procedures with foot washing (where the operation was performed) are only possible after removal of the stitches;
- saunas, baths and hot tubs are prohibited during the healing period;
- Postoperative analgesics are prescribed by a doctor. Self-election is forbidden;
- are taking additional medicines to prevent blood clots;
- taking medications to strengthen the walls of blood vessels (vitamins E and C);
- It is forbidden to stay standing / sitting for a long time in high heels and tight underwear;
- During the rest period, the legs should be above body level. It promotes the outflow of excess blood and reduces swelling;
- Introduce physical activity in a timely and gradual manner to normalize blood flow (discussed with your doctor);
- massages and physiotherapy are performed with the permission of the treating specialist;
- Refusal of alcoholic beverages and nicotine. Alcohol causes vasodilation, and tobacco, on the contrary, leads to narrowing. These effects reduce the efficiency of the operation;
- if you are prescribed an overweight, low-calorie diet.
If the rules are followed, full recovery of limb function is possible within 6 months.
Laser endovenous coagulation
Laser removal of veins with varicose veins is performed when direct vessels with a diameter of at least 0. 02 cm are touched and there are few capillaries. The procedure consists of light waves acting on damaged vessels by soldering and destroying them.
Equipment
Laser coagulation of veins can be performed with any of 3 types of optical fiber:
| Optical Fiber Type | Short Action |
| End (classic) | This creates a light guide radiation from the end, meaning the vessel is closed in front of it. Disadvantages include the development of hematomas and a tight feeling in the veins. The maximum diameter of the vein is 0, 1 cm. |
| Radial (painless radial light guide with elves) | The light waves in the fiber form a circle that surrounds a vein of diameter. This allows the treatment of veins of any size. The risk of developing a hematoma and swelling is also minimized. |
| Made of 3 types of radial optical fiber | Two light ring lasers are used to eliminate the varicose veins. The first prepares the vein for the procedure (eliminates excess fluid), the second round solders the walls. For treatment, light guides are produced for fine and short veins as well as large vessels. |
The equipment is chosen not only by the patient but also by the vascular condition specialist.
Which veins can be removed using the EVLK method
Before a phlebologist (a specialist who examines veins and eliminates varicose veins) chooses EVLK, the characteristics of the damaged blood vessels must be determined. They must be straight and at least 2 mm in diameter.
As a result, laser therapy can be applied to the following vascular groups:
- small and large saphenous vessels;
- saphenous accessory veins at least 5 mm from the surface of the epidermis;
- vessels that connect the deep veins to the superficial vessels.
For other veins, therapy is only possible with phlebectomy.
Efficiency
Veins can be removed by EVLK using 3 types of optical fiber. The effectiveness of the treatment varies depending on the type of equipment. When an operation is performed with the help of an end light guide, the effectiveness of the therapy is 94-96%. Working with radial light guides allows you to achieve 100% results in eliminating varicose veins on your legs.
Stages of preparation and implementation
When choosing to remove varicose veins using EVLK, the patient should undergo the following training:
- Deletion of hormonal drugs (if taken). Because they can cause thrombosis;
- blood thinners should be taken one day before the procedure;
- screening of damaged veins to determine the extent of damage;
- Perform tests to rule out the presence of latent infection or inflammatory processes in the body. Blood clotting is also determined;
- The area of the procedure is thoroughly washed and shaved (only antibacterial soap is allowed without the use of cosmetics).
Before starting the operation, the boundaries of the damaged vessels, the location of the laser / fiber insertion, and the location of the branching capillaries are marked. These marks make it possible to solder the beginning and end of the vein and the outlet of the capillaries. The process is performed under the control of an ultrasonic device.
EVLK is made in stages:
- Insert the catheter through a small puncture (the catheter insertion site is anesthetized with local anesthesia) in the indicated area. The light guide will move through it.
- Insert the light guide into the catheter and advance it to the injured area. Ultrasound control, monitor.
- Anesthetic injection to numb the vein and adjacent tissues.
- Advancement of the "active" light guide through the damaged vein, followed by a delay at the sites of capillary bifurcation (to close the outlets and prevent bleeding).
- Remove the laser by antiseptic treatment of the puncture site and tightening the elastic bandage (or using a compression stocking).
The patient can leave the hospital immediately after completing the procedure.
Features of rehabilitation
To restore the function of the injured limb and prevent complications, you should be familiar with the nuances of rehabilitation after EVLK.
They are:
- After completing the procedure, it is recommended to walk the operated leg for one hour in the medical institution;
- Ultrasound adjustment of the treated vein is performed for 2-3 days;
- You must wear special underwear for 5 days a day (the type of stockings will be discussed with your healthcare professional before surgery). Then wear day clothes within 45-60 days;
- Knead your legs daily by walking every day for 60 minutes;
- Avoid overloading your legs (prolonged sitting or standing position), taking a sauna, or taking a hot bath.
If it is still necessary to remove the varicose vein, the procedures can be performed no earlier than 7 days later.
Benefits of each method
Depending on the type of procedure, varicose vein surgery has the following benefits:
| Phlebectomy | EVLK |
| The incision is about 5 mm, so there is little scar left | No pain during the procedure (using local anesthesia). General anesthesia is not required |
| Painless as surgery is performed under local anesthesia. Local anesthesia is used for miniflebectomy. | is done with EVLK ultrasound control. The result is high accuracy and efficiency. |
| Low cost | Hematoma and pain at the site of surgery are rare or mild. |
| Quick restoration of skin tone (lack of stars and purple-cyanotic hue of the epidermis) | This operation requires 1 puncture, so no stitches or scars are required |
| Short recovery period of about 30 days | Recovery time up to 5 days |
| Effective for all forms of varicose veins | After surgery, the patient can leave the clinic within 1 hour. |
| Return to normal life is possible within 24 hours. | |
| EVLK can be performed when the integrity of the epidermis is compromised by ulcers. | |
| The maximum duration of surgery is 40 minutes. | |
| EVLK can be done in one day on both days. A second operation on one leg is allowed after 7 days. |
The risk of infection during the procedure is minimal as the incision / puncture is small.
Complications after surgery and laser venous surgery
There is a risk of complications after surgical or laser removal of veins. Negative reactions may occur due to low training of the professional or violation of the rules during the rehabilitation period. Possible complications of phlebectomy and endovenous coagulation.
| Vein Removal Methods | Minor complications from procedures | Serious complications |
| Phlebectomy |
|
|
| Endovenous laser coagulation |
|
|
An allergic reaction to anesthetics may occur during both procedures.
Measures to minimize complications
Surgery to remove varicose veins sometimes involves complications that are needed to prevent them from appearing:

- examination of allergic reactions to the drugs used;
- exclusion of infectious diseases and inflammatory processes in the body before surgery;
- selection of proven clinics with highly trained professionals and modern equipment;
- compliance with the rules during the recovery period. He especially wears compression underwear;
- Observe dietary foods during the recovery period (discussed by a specialist after the procedure). The amount of pure water in the diet increases, the food is ingested in small portions, the diet is enriched with vitamins and minerals;
- resting feet during working hours;
- surgery should be performed after surgery to monitor the dynamics of limb repair;
- to perform massages and physiotherapy to quickly restore blood flow.
If you find unacceptable discrepancies during the operation, you should contact the clinic immediately.
Compare forecasts
With both methods of leg vein removal, the probability of complete recovery is greater than 95%, but to eliminate contraindications, follow the rules during the rehabilitation period, and select a proven clinic. With surgical treatment, blood flow and the external condition of the legs are restored after 3 months, and with laser therapy, healing can be seen after 30 days.
In an advanced form, the removal of blood vessels is performed by surgery. The mode of treatment is determined not only by the patient's desire, but also by the presence of indications and contraindications to the procedure. The effectiveness of therapy depends on the doctor's qualifications and the implementation of postoperative foot care rules.























